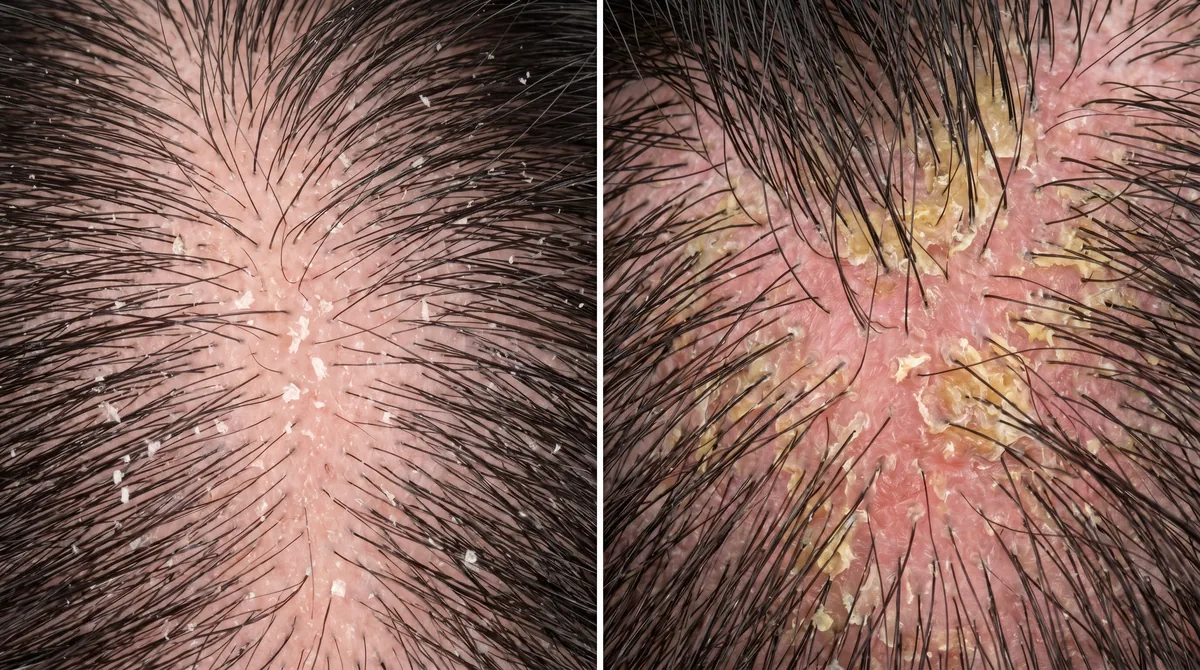
You’ve been dealing with flakes for months. You’ve tried every anti-dandruff shampoo at the pharmacy. Nothing works for more than a few days. Here’s the thing: what you’re treating as dandruff might actually be seborrheic dermatitis, a chronic inflammatory condition that requires a completely different approach.
The two conditions look similar at first glance. Both cause flaking. Both affect the scalp. But seborrheic dermatitis is persistent, inflammatory, and won’t respond to basic dandruff treatments. Misdiagnosing one for the other means you’re using the wrong products and getting frustrated when they don’t work.
This article contains affiliate links. See our affiliate disclosure for details.
In the Gulf region, hard water compounds both conditions by changeing your scalp’s natural pH balance and creating a mineral layer that traps sebum and dead skin cells. Understanding which condition you’re dealing with is the first step toward finding a treatment that actually works.
The Core Difference: Inflammation vs Irritation
Dandruff is a mild scalp condition caused by sensitivity to a naturally occurring yeast called Malassezia. Your scalp sheds skin cells faster than normal, creating those familiar white flakes. It’s annoying but not inflammatory.
Seborrheic dermatitis is a chronic inflammatory skin disorder. Yes, Malassezia plays a role here too, but your immune system overreacts to it, triggering inflammation. The result isn’t just flaking. It’s red, irritated patches with greasy-looking yellowish scales that can spread beyond your scalp to your eyebrows, sides of your nose, and even your chest.
The distinction matters because anti-inflammatory treatments (like ketoconazole or corticosteroid shampoos) work for seborrheic dermatitis but are overkill for simple dandruff. Meanwhile, basic dandruff shampoos won’t touch the inflammation driving seborrheic dermatitis. You can’t treat inflammation with exfoliation alone.
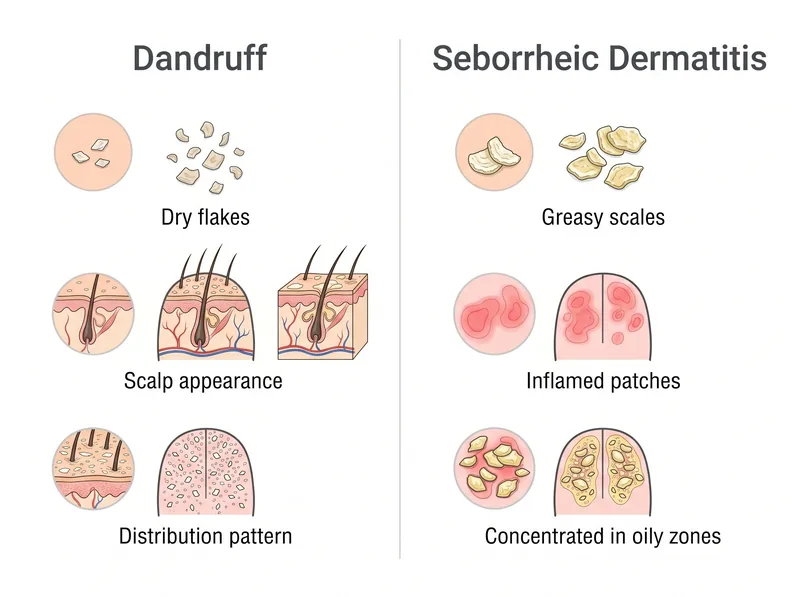 Key visual differences between seborrheic dermatitis and simple dandruff
Key visual differences between seborrheic dermatitis and simple dandruff
Visual Symptoms: What You’re Actually Seeing
Dandruff flakes are small, white, and dry. They fall onto your shoulders like snow. Your scalp might feel slightly itchy, but it looks relatively normal, maybe a bit pink, but not inflamed. The flakes brush off easily and don’t stick to your hair.
Seborrheic dermatitis flakes are larger, yellowish, and greasy. They stick to your scalp and hair. Underneath those flakes, your scalp is visibly red and inflamed, often in patches concentrated around your hairline, behind your ears, or in the oilier zones of your scalp. The affected areas might feel tender or burn slightly.
If you’re seeing redness that persists even after washing, or if the flakes have a yellowish, oily appearance, you’re likely dealing with seborrheic dermatitis. A study published in the Journal of Clinical and Aesthetic Dermatology found that 50% of adults misidentify seborrheic dermatitis as simple dandruff and delay proper treatment by an average of six months.
Another telltale sign: seborrheic dermatitis often appears in other sebum-rich areas. Check your eyebrows, the creases beside your nose, and your upper chest. Dandruff stays on your scalp.
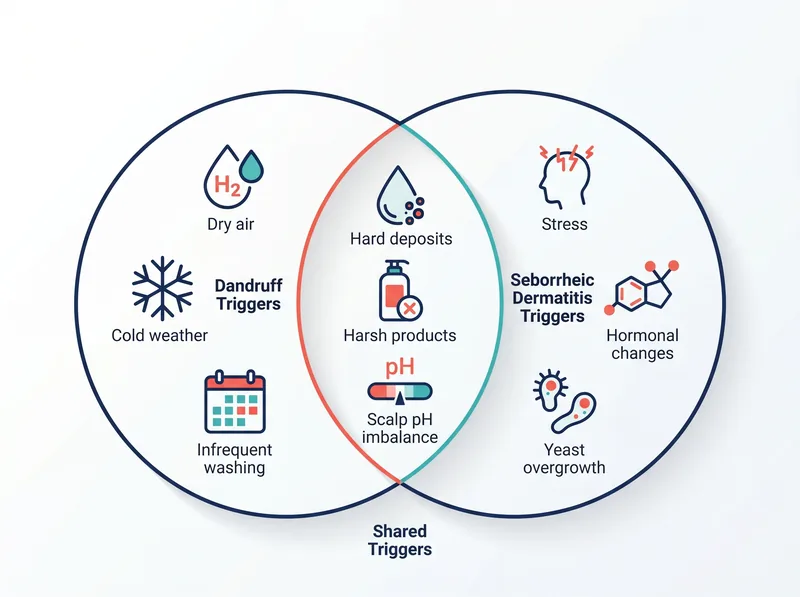 Common triggers differ between the two conditions, though some environmental factors affect both
Common triggers differ between the two conditions, though some environmental factors affect both
Triggers and Aggravating Factors
Dandruff flares when your scalp is too dry or when you’re not washing frequently enough. Cold weather, low humidity, and harsh shampoos that strip natural oils all make it worse. It’s a mechanical problem: your scalp is shedding faster than it should.
Seborrheic dermatitis has different triggers. Stress is a major one, many people notice flares during high-pressure periods. Hormonal shifts, lack of sleep, and even certain medications (like lithium or interferon) can trigger episodes. The condition is also linked to neurological disorders; people with Parkinson’s disease have significantly higher rates of seborrheic dermatitis.
Both conditions get worse in the Gulf’s hard water environment. The high mineral content changes your scalp’s pH balance, creating an environment where Malassezia yeast thrives. The mineral buildup also forms a barrier that traps sebum and dead skin cells, making both dandruff and seborrheic dermatitis harder to manage. This is why many Gulf residents notice their scalp issues started or worsened after moving to the region, as discussed in our article on hair problems after relocating.
For seborrheic dermatitis specifically, anything that increases sebum production makes things worse. That includes high-fat diets, alcohol consumption, and even some B-vitamin deficiencies. Research from the American Academy of Dermatology shows that people with seborrheic dermatitis often have altered lipid compositions in their skin, making them more susceptible to yeast overgrowth and inflammation.
Treatment Approaches That Actually Work
For dandruff, zinc pyrithione or selenium sulfide shampoos usually do the trick. Use them 2-3 times per week, leaving the lather on for 3-5 minutes before rinsing. Between treatments, use a gentle, pH-balanced shampoo. Most people see improvement within two weeks.
Seborrheic dermatitis requires a more aggressive approach. Ketoconazole 2% shampoo is the gold standard, it’s both antifungal and anti-inflammatory. Apply it to affected areas, leave it on for 5-10 minutes, then rinse thoroughly. You’ll typically use it twice weekly initially, then taper to once weekly for maintenance.
But here’s what dermatologists don’t always mention: if you’re dealing with hard water, medicated treatments can’t penetrate the mineral buildup on your scalp. That’s where a chelating shampoo like Regrowth+ becomes useful. Use it once weekly to remove the mineral layer, creating a clean surface for your medicated treatments to work. Think of it as prep work before the real treatment.
For severe seborrheic dermatitis, your dermatologist might prescribe a topical corticosteroid for short-term use to calm acute inflammation. These work fast but can’t be used long-term due to side effects like skin thinning. The goal is to knock down the inflammation quickly, then maintain control with antifungal shampoos and proper scalp care.
Don’t forget the basics. Wash your hair regularly, seborrheic dermatitis thrives when sebum and dead skin accumulate. Manage stress through whatever works for you (exercise, meditation, adequate sleep). And if you’re in the Gulf, consider the environmental factors outlined in our guide on hard water’s impact on hair health.
When to See a Dermatologist
If over-the-counter dandruff shampoos haven’t worked after four weeks, stop guessing and see a dermatologist. Persistent flaking despite treatment is the clearest sign you’re dealing with something beyond simple dandruff.
Other red flags: spreading redness, flakes that appear yellowish or greasy, symptoms in areas beyond your scalp (eyebrows, face, chest), or any oozing or crusting. These all point to seborrheic dermatitis or potentially another condition entirely, like psoriasis or contact dermatitis.
Seborrheic dermatitis can also signal underlying health issues. It’s more common in people with weakened immune systems, neurological conditions, or certain nutritional deficiencies. If you’re experiencing other unexplained symptoms alongside your scalp issues, mention them to your doctor.
A dermatologist can perform a simple visual examination to differentiate between dandruff and seborrheic dermatitis. In rare cases where the diagnosis isn’t clear, they might do a scalp biopsy or fungal culture. But usually, the clinical presentation is obvious to a trained eye. Don’t spend months trying random products when a 15-minute appointment could give you a definitive answer and proper treatment plan.
Long-Term Management and Prevention
Dandruff can often be controlled and eventually eliminated with consistent treatment. Once you find a shampoo that works, use it regularly for a few months, then you might be able to switch to maintenance mode or stop treatment altogether.
Seborrheic dermatitis is chronic. It comes and goes. Even with perfect treatment, you’ll likely have flares during stressful periods or seasonal changes. The goal isn’t to cure it, it’s to keep it controlled and minimize flare-ups.
For both conditions, scalp hygiene is non-negotiable. That doesn’t mean washing daily with harsh shampoos. It means regular cleansing with appropriate products, thorough rinsing (especially important in hard water areas), and avoiding heavy styling products that build up on your scalp.
Pay attention to your triggers. Keep a simple log for a month: note when flares happen and what preceded them. Stress? Dietary changes? Weather shifts? Pattern recognition helps you prevent flares before they start. And if you’re in the Gulf, water quality is almost certainly a factor worth addressing through filtration or chelating treatments.
References
- Seborrheic Dermatitis: Etiology, Risk Factors, and Treatments - Journal of Clinical and Aesthetic Dermatology
- Seborrheic Dermatitis: Overview - American Academy of Dermatology
- The Role of Malassezia in Seborrheic Dermatitis - PubMed Central
- Treatment of Seborrheic Dermatitis - American Family Physician